 Liposuction to treat lipedema (abnormal build-up of fat in your legs and arms, causing pain or limiting movement).At least two medically necessary reasons might qualify. The steps for getting health insurance to pay for liposuction are the same for Medicaid, as this publically-funded program follows similar claims underwriting rules. Include the appropriate ICD-10 and CPT codes and the prognosis or expected outcome.įor example, Medicaid might cover liposuction if you can establish a medically necessary reason upfront for this plastic surgery to harvest fat from targeted areas on your body.Address how it treats a disease or illness and why it is consistent with the applicable standard of care.The requesting physicians should submit documentation to the Managed Care Organization (MCO) or state agency for pre-certification, including photographs, measurements, chart records, and any other evidence supporting the specific diagnosis. Taxpayer funding of the program does not alter the claims underwriting process. The steps for getting health insurance to pay for plastic surgery are the same for Medicaid. These procedures are medically necessary your surgeon must submit documentation before the operation for pre-certification. Medicaid often covers plastic surgery that reconstructs facial and body defects or treats an illness, injury, or symptoms. Medicaid coverage for excess skin removal.Of course, you must prove the operation meets precise criteria in these examples and others. 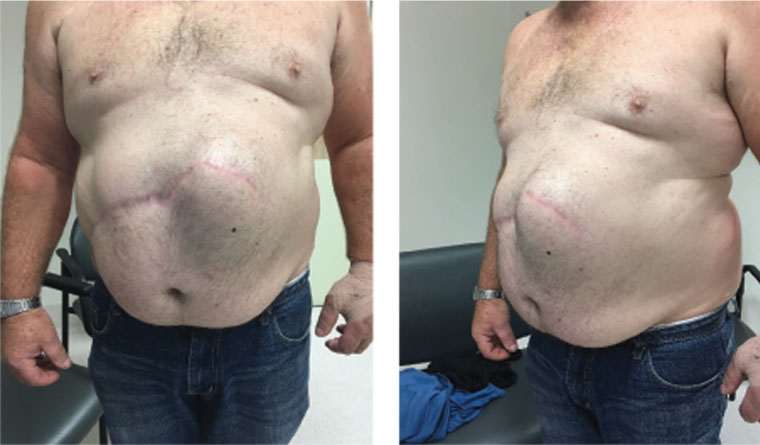
Medicaid often pays for plastic surgery deemed medically necessary or reconstructive – even when the procedure improves appearance. Medicaid might pay for the anesthesia, nurses, operating room, and other shared expenses while rejecting claims connected exclusively to cosmetic services. The closure of separated abdominal muscles after pregnancy typically falls into the cosmetic surgery category because it addresses appearance, not function.įinancial help paying for surgery might come by combining the Diastasis Recti procedure with a medically necessary one, such as an umbilical hernia repair. You have not established a consumer report with six months of payment history.įor example, getting Medicaid to cover Diastasis Recti will be challenging unless you can identify a creative workaround.Your credit report contains adverse payment history (charge-offs, bankruptcy, etc.).This approach might fit if you fall into one of these categories. 
No credit check cosmetic surgery financing might help low-income patients unable to get a loan or payment plan through traditional channels. Therefore, low-income patients seeking to improve their appearance might need another way to pay for the operation. Medicaid does not cover cosmetic surgery unless the procedure is medically necessary. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
